Tooth decay almost never starts with pain. It starts with a quiet change on the surface. A tiny mineral loss. A place where plaque sits a little longer. A spot that gets hit by acid again and again. And because it’s quiet, people wait. They tell themselves it’s “just sensitivity” or “I’ll book the dentist soon.”
Then one day they’re standing in a pharmacy aisle at 9 p.m., buying the strongest numbing gel they can find, chewing on one side like a nervous squirrel, and wondering why the ache feels like it has its own heartbeat.
Here’s the thing: “rotting teeth” isn’t a medical label. Dentists call it tooth decay or dental caries. But the everyday phrase isn’t wrong. A tooth can break down in steps, moving from enamel damage to a deep infection that can spread past the tooth. Mayo Clinic puts it plainly: cavities are damaged areas that turn into holes, and they can lead to toothache, infection, and tooth loss.
This article walks through the real rotting tooth stages the way they actually play out, what speeds them up, what signs people miss, and what to do before it turns into a full-blown mess.
How Teeth Start Falling Apart In The First Place
Teeth don’t “go bad” overnight. They get worn down by acid, over and over.
Plaque is the main troublemaker. It’s that sticky film that adheres to teeth. Bacteria that live in plaque feast on carbs and sugars. Then they make acids. Those acids draw out minerals from enamel, the hard outer layer of the tooth. That early mineral loss is why you’ll occasionally see a white, chalky spot first. This basic sequence chain is explained plainly by the National Institute of Dental and Craniofacial Research: bacteria produce acids that dissolve enamel, which causes a cavity.
Now add real life.
People snack all day. People sip drinks for hours. People fall asleep watching Netflix and forget to brush. And in 2026, dentists keep pointing out a few “modern life” habits that quietly raise risk:
-
Sip all day habit: energy drinks, soda, sweet coffee, sports drinks, even lemon water. It’s not just sugar. Acid plus time matters. If teeth stay bathed in acid, enamel can’t recover between hits. Mayo Clinic calls out frequent snacking and sipping sugary drinks as a cavity driver.
-
Starchy snacking: chips, crackers, pretzels. They break down into sugars and get packed between teeth. They hang around longer than people think.
-
Dry mouth: Saliva is a natural rinse. When saliva drops, decay risk climbs. The American Dental Association has a whole dry mouth guide and notes that fluoride measures can help protect teeth when saliva is low.
And yes, brushing and flossing matter. But the timing and patterns matter, too.
The Rotting Tooth Stages People Actually Move Through
Let’s walk it from the first quiet warning to the big, painful finale.
Read Also: The Honest Truth About Fixing Your Shakes: How to Make Protein Powder Taste Better
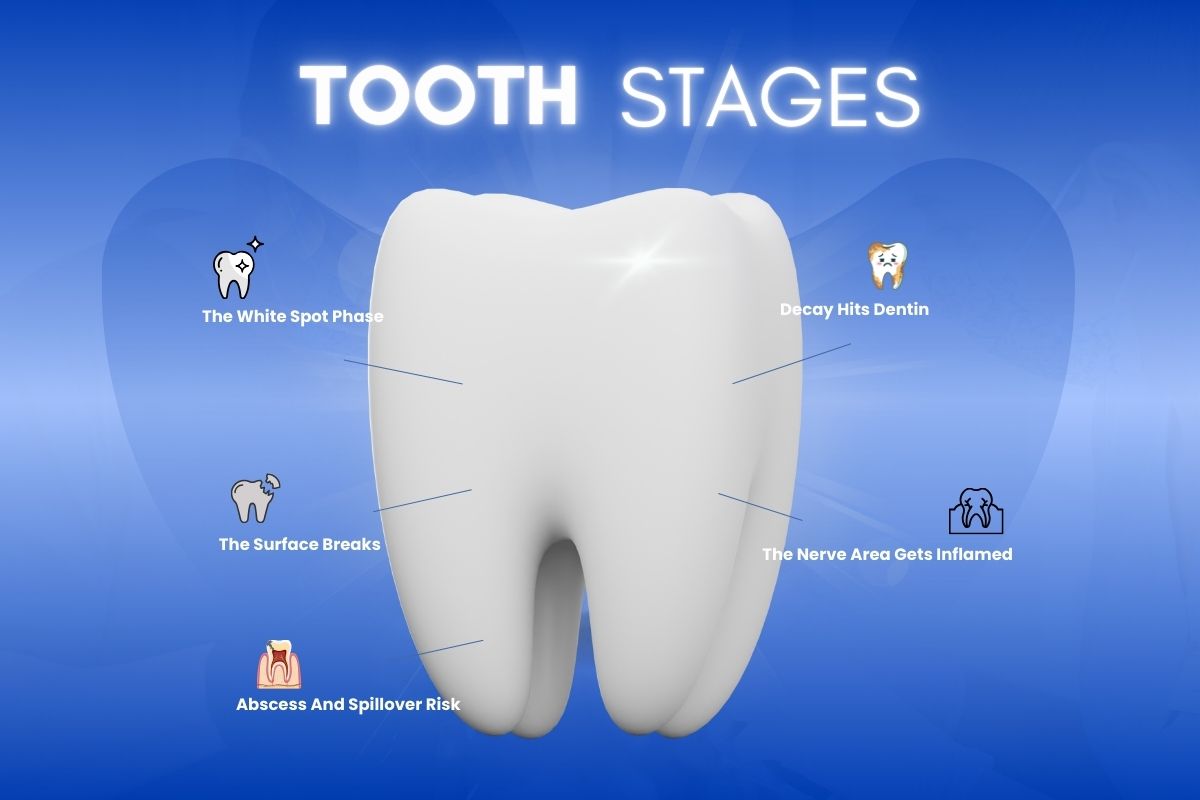
Stage One: The White Spot Phase
This is enamel losing minerals. You might not feel anything. You might see a chalky patch, usually near the gumline or in grooves on chewing surfaces. Johns Hopkins describes white spots as an early sign that enamel is starting to break down.
At this stage, a dentist may talk about fluoride, better cleaning, and changing what you sip and snack on. This is the window where you can sometimes stop the slide and strengthen enamel again.
Stage Two: The Surface Breaks
Once enamel collapses and a hole forms, that spot can’t “grow back”. The tooth has a cavity now, even if it’s tiny. The color may shift from white to light brown or yellow. Johns Hopkins notes that early cavities can look light brown and then darken as they deepen.
A filling is the common fix here. The dentist removes the decayed part and seals the opening.
Stage Three: Decay Hits Dentin
Under enamel sits dentin. It’s softer. It has tiny tubes that connect to the nerve area. So when decay reaches dentin, things often speed up. This is when many people finally notice sharp sensitivity to cold, heat, or sweets.
You might bite down on ice cream and feel a quick sting that makes your eyes water. Or you might drink something hot and get that jolt. This stage often needs a bigger filling, and sometimes a crown if the tooth has lost a lot of structure.
Stage Four: The Nerve Area Gets Inflamed
Inside the tooth is the pulp, where nerves and blood vessels live. When bacteria reach that space, pain often turns from “annoying” to “can’t sleep”. Throbbing. Pressure. Pain that spreads into the jaw or ear.
At this stage, a root canal is often the tooth-saving option. It removes infected pulp, cleans the inside, and seals the tooth.
Stage Five: Abscess And Spillover Risk
This is the part nobody wants. An abscess is a pocket of pus from an infection. It can form near the root tip or in the gums. According to the Cleveland Clinic, a tooth abscess is a pus pocket caused by bacteria that begins as an infection. It also says it can spread to the surrounding bone and neighboring teeth.
The symptoms may include swelling, fever, an unpleasant taste, radiating pain, and general malaise. Mayo Clinic’s abscess page cautions that if the infection isn’t treated, it can spread. Some dentists may still be able to perform a root canal at this stage, but extraction is also common when the tooth is not salvageable.
So, How Long Does It Take For Teeth To Rot Away?
People ask this like there’s a stopwatch. There isn’t.
Some cavities creep along for years. Some move fast, especially once dentin gets involved. What changes the speed?
-
Frequent sugar or acid exposure. Not the size of one dessert, but the number of “hits” per day.
-
Low saliva from dry mouth, which can happen with many meds and health conditions.
-
Deep grooves in teeth that trap plaque.
-
Past decay history. If you’ve had cavities before, your risk tends to run higher.
-
And honestly, access to care matters. The CDC notes cavities are common and can go untreated, which is when pain and infections show up.
If you want a plain answer: early enamel changes can show up faster than people expect, but a tooth “rotting away” is usually the result of months or years of repeated damage, plus delay.
Signs People Miss Until It’s Too Late
Early signs can be subtle:
-
A chalky white patch on enamel
-
Bad breath that keeps coming back
-
A rough spot you feel with your tongue
-
Mild cold sensitivity that comes and goes
Later signs are loud:
-
Pain when chewing
-
Lingering sensitivity after a hot or cold
-
A visible hole or dark spot
-
Swelling near the tooth or gum
-
A bad taste that shows up out of nowhere
-
Pain that wakes you up at night
The annoying truth: pain can arrive late. Some people don’t feel much until the decay is deep.
What Tooth Decay Can Do To The Rest Of The Body
Read Also: Why Your Back Hurts and What Yoga Can Do About It
Most cavities stay local if you treat them early. But deep infections can become a bigger deal.
An abscess can spread into nearby tissues and bone. In rare cases, serious infections can move beyond the mouth and become dangerous. Public health guidance often warns about this risk when decay is not treated.
I’m going to keep this grounded: most people with cavities won’t get a life-threatening complication. But if you have facial swelling, fever, or trouble swallowing, or you feel weak and sick, that’s not “normal tooth pain”. That’s a get-help-now situation.
Can Tooth Decay Cause Diarrhea?
Directly, not usually.
A simple cavity typically won’t cause diarrhea. But a severe tooth infection can make people feel generally ill, with nausea or vomiting in some cases. According to WebMD, dental abscesses are capable of inducing some combination of nausea and/or vomiting in association with fever-like symptoms.
Diarrhea can also come on for other reasons around the same time — perhaps antibiotics, stress, a change in diet or an acute stomach bug. If diarrhea is accompanied by a fever, swollen face and an exacerbating tooth infection, that combination needs medical attention. Not a wait-and-see.
How Dentists Figure Out The Stage
Dentists look, probe gently, and ask the right questions. They also use X-rays to see between teeth and check how deep a cavity goes.
Early enamel changes can be hard to spot at home, which is why routine checkups catch issues before pain forces the visit. The CDC keeps stressing how common cavities are and how often people live with them for a long time.
Treatment That Matches The Damage
Early enamel damage: fluoride, better daily cleaning, changes to sipping and snacking patterns. Sometimes sealants, depending on the tooth and risk.
-
Small to medium cavities: fillings.
-
Big cavities with weak tooth structure: crowns.
-
Infected pulp: root canal plus restoration.
-
Abscess or severe breakdown: root canal or extraction, sometimes paired with antibiotics when infection has spread, or risk is high.
No hype here. The sooner you treat it, the simpler it usually is.
Keeping Teeth From Getting To That Point
-
Brush twice daily with fluoride toothpaste.
-
Clean between teeth daily. That’s the base.
But if you want the real-life upgrade, it’s this:
-
Stop feeding bacteria all day long.
-
Try to keep snacks and sweet drinks at set times, not stretched across hours.
-
Water between.
-
Give enamel a break.
If you deal with dry mouth, bring it up at dental visits. There are targeted fluoride options and practical steps that can help protect enamel when saliva is low.
Quick FAQs People Always Ask
What is Stage 1 of rotting teeth?
It’s usually the white spot phase, when enamel is losing minerals, but there’s no hole yet.
How long does it take for teeth to rot away?
It depends on diet patterns, saliva level, cleaning habits, tooth shape, and whether you get care early. There’s no single timeline that fits everybody.
Can tooth rot reverse on its own?
Early mineral loss can sometimes be stopped and strengthened. A true hole in enamel won’t heal back into a solid tooth.
When should you see a dentist fast?
If pain keeps you up, swelling shows up, you have a fever, or swallowing feels hard, don’t wait.
Final Word
Tooth decay is mostly boring. Until it isn’t.
It starts as a quiet chemical process. A little acid. A little plaque. A small change in enamel. And if you catch it there, it’s often a simple fix.
If you ignore it, the tooth doesn’t “get better”. It usually gets more expensive, more painful and way more annoying. And at some point, you stop thinking about the tooth and start thinking about your entire face.
So, for real: if you had to bet on it, are you in the early stage … or are you already bargaining with yourself about making the appointment next week?
Sources and References
-
Mayo Clinic. Cavities and Tooth Decay: Symptoms and Causes
-
Mayo Clinic. Tooth Abscess: Symptoms and Causes
-
Centers for Disease Control and Prevention (CDC). Cavities and Tooth Decay Facts
-
National Institute of Dental and Craniofacial Research (NIDCR). Tooth Decay
-
Johns Hopkins Medicine. Tooth Decay and Cavities
-
American Dental Association (ADA). Xerostomia (Dry Mouth)
-
Cleveland Clinic. Tooth Abscess
-
WebMD. Dental Abscess Guide












